AI in Electronic Health Records
In 2023, the government issued a mandate for the digital transformation of the NHS, stipulating that 95% of trusts must adopt electronic health records (EHRs) by March 2025. This was the natural next step to ensure the NHS stays at the forefront of clinical practice and system operations.
For many, the transition to EHRs marks a significant improvement over traditional paper-based systems. EHRs enhance user accessibility, streamline clinician communication, and ensure continuity of care, thereby facilitating better-informed decision-making. They also enabled unprecedented research using the vast amounts of captured data. However, in recent years, there has been a growing recognition of the unintended consequences of EHRs, particularly their contribution to clinician burnout.
Clinician burnout
Burnout primarily arises from the increase in administrative tasks and the cognitive load they impose on clinicians. Poor user interfaces and excessive documentation requirements, often driven by regulatory demands, exacerbate this problem.
For instance, a study found that clinicians can spend over two hours a day on electronic health records OUTSIDE of normal working hours. That 9-5 quickly becomes 9-7.
Another factor that has fueled this fire is remote access. The availability of EHRs on laptops and even smartphones (such as EPIC and soon Cerner), means clinicians are perpetually connected to their work. This constant connectivity is akin to a professional form of doom scrolling.
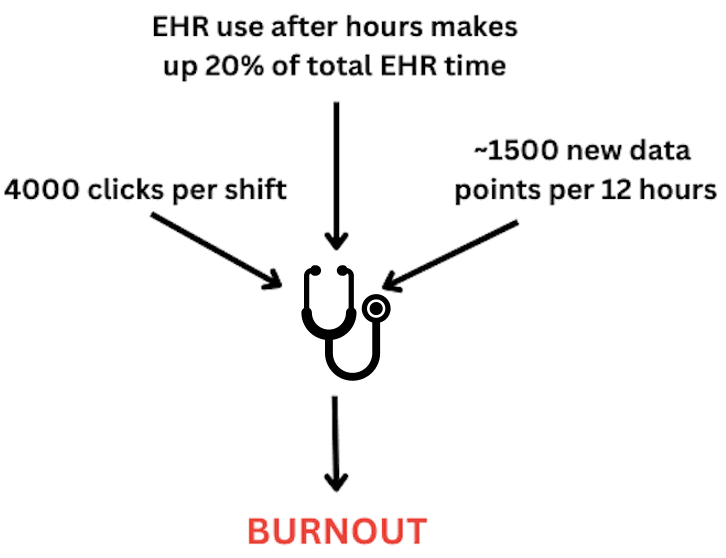
Let me take on a ward round
“Hi patient X how are you” Bleep from nurse in charge “ward round not documented” Bleep from site manager “discharge summaries not completed” Bleep from pharmacy “regular medications not transcribed” Sounds familiar?
Clinicians are expected to review patients whilst simultaneously juggling a multitude of administrative tasks. Junior doctors, in particular, often bear the brunt of this burden, feeling detached from clinical medicine and missing valuable training and teaching opportunities due to the overwhelming pressure to prioritise administrative duties.
We need help!
Let’s go AI
The integration of AI into clinical workflows has the potential to completely change how we interact with electronic health records. By automating mundane and repetitive administrative tasks, AI can free up clinicians to focus on what truly matters: patient care.
Every day, up to 70,000 people visit A&E or walk-in centers in the UK, each requiring a discharge summary. Why not leverage AI to generate these summaries? This would be one example where AI can significantly reduce the administrative burden on clinicians.
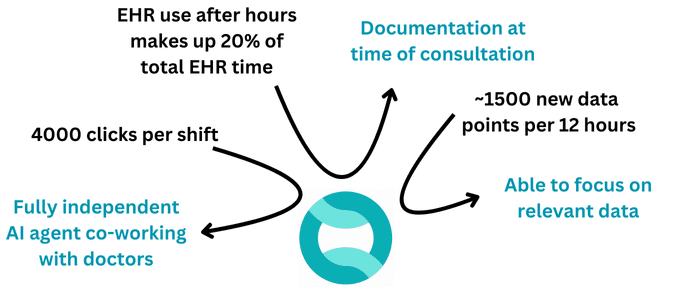
AI co-pilots will act as the first barrier of defense for clinicians against EHR overload. At Tortus, we’re building the world’s first completely digital healthcare team member
Insights from Experts: Dr. Ellie Asgari weighs in
During my recent conversation with our very own Clincian-in-Residence Dr. Ellie Asgari, we delved into the transformative impact of AI technologies in healthcare.
‘The integration of AI, particularly large language models within EHRs, is already making significant strides. AI assistants can automate tedious tasks such as capturing and summarizing patient encounters, generating discharge and outpatient letters, creating preliminary reports, and populating progress notes with pre-defined templates. Additionally, AI can streamline tasks like appointment scheduling, medication order entry, and referral generation by learning a clinician's preferences and automating repetitive aspects of these processes. This frees up valuable time for clinicians to focus on what matters most: providing high-quality, personalised care to their patients.
However, while AI integration in EHRs offers exciting possibilities for reduced workload, doctors must remain vigilant in ensuring the accuracy of AI outputs and safeguarding patient safety!’
If you’re interested in learning more about the relationship between EHRs, cognitive load, and burnout, check out our recently published review (available for free on PubMed)
TORTUS is committed to being net zero by 2050
TORTUS AI LTD
14487060
5 Brayford Square
E1 0SG
© TORTUS AI. All rights reserved